Please note that the information on this page relates specifically to complaints regarding accident & health claims.
For WORKERS COMPENSATION COMPLAINTs, please use our feedback form.
Complaints and Dispute Resolution
EML manages claims on behalf of a number of insurers. Despite our best efforts to manage all claims promptly and fairly, we acknowledge that sometimes complaints or disputes do occur. When this happens, we take your concerns seriously and aim to find a resolution that's fair for all parties.
At any time during the claim process you can access our comprehensive complaint handing and dispute resolution process. This service is free of charge to policyholders and claimants.
What to do if you have an accident & health complaint
If you have a complaint or experience dissatisfaction with our service or decision regarding your claim please contact us immediately.
You may contact your EML Case Manager and advise this person of your particular dissatisfaction and that you wish to have it rectified. In most cases, complaints are immediately resolved.
If you wish to formalise your complaint, please contact us at:
|
EML GPO Box 4580 Sydney NSW 2001 Email: info@eml.com.au
|
Please provide us with as much information and supporting documentation as possible, as well as the reason for your complaint.
An EML representative will respond to your complaint in writing 10 business days.
If we require further information or further assessments or investigations, we will notify you of what is required and will keep you informed of the progress of your complaint every 10 business days.
If the response from EML resolves your complaint, you will receive confirmation in writing acknowledging finalisation of your complaint.
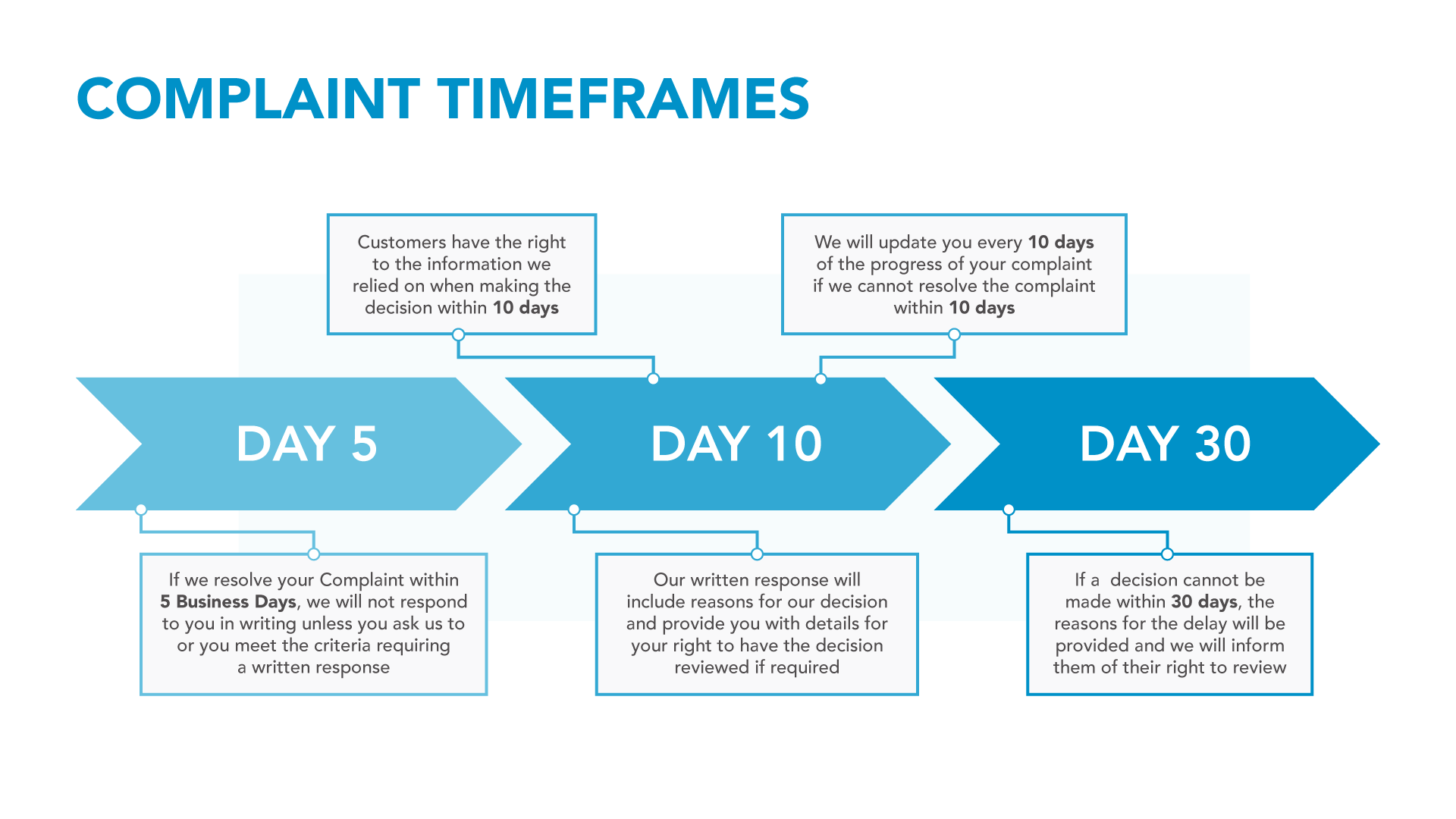
Complaint Timeframes
What to do if your complaint is not resolved
If, after receiving the response from EML, your complaint is not resolved, or if you are not satisfied with the way your complaint was managed by EML, you will be provided with your insurer contact details as part of the decision advised to you by EML.
Keeping you informed
Your complaint will be acknowledged in writing. You will be informed of the progress of your complaint within 10 business days. You will be provided with the name and contact details of the person assigned to reviewing your complaint and they will do their utmost to resolve the complaint to your satisfaction, within 10 business days.
If your complaint cannot be resolved within 10 business days, you will be provided with an update every 10 business days, unless you agree to a different timeframe.
You will be provided with a final decision and the information relied upon when making the decision, within 30 calendar days of the date on which you first made your complaint.
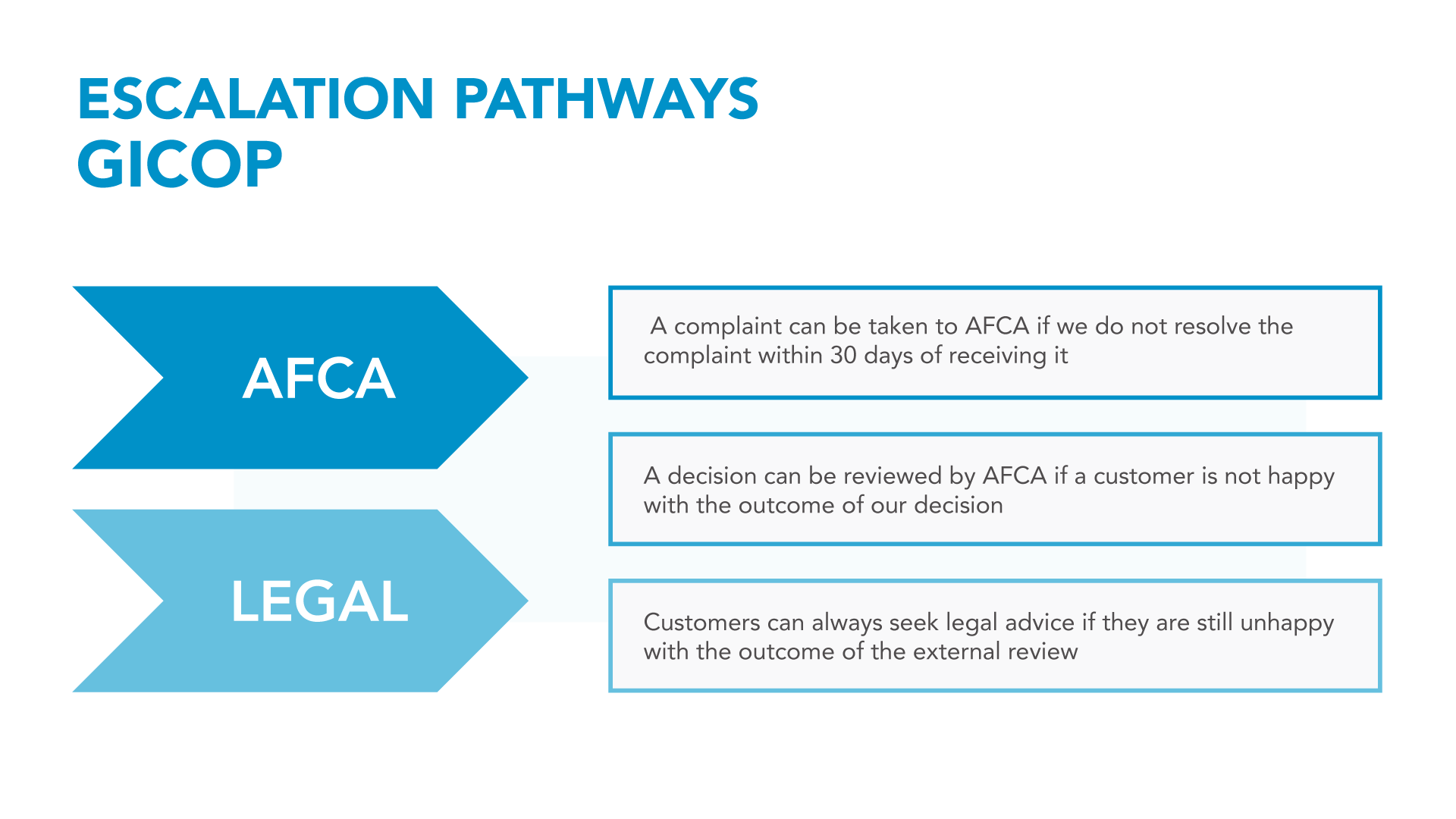
If your complaint is still not resolved
If your complaint is not resolved within 30 calendar days, you will be advised in writing the reasons for the delay. If your complaint is not resolved in a manner satisfactory to you, you may refer the matter to the Australian Financial Complaints Authority (AFCA). Your dispute must be referred to AFCA within 2 years of the date of the insurer's final decision.
Our insurers are members of the AFCA external dispute resolution scheme and agree to be bound by its final determinations about a dispute.
AFCA can be contacted by mail, telephone and email at:
|
Australian Financial Complaints Authority GPO Box 3 Melbourne Vic 3001 Telephone: 1800 931 678 Email: info@afca.org.au |
Clients not eligible for referral to AFCA, may be eligible for referral to the Financial Ombudsman Service (UK). Such referral must occur within 6 months of the final decision by the Complaints team at Insurer. Further details will be provided to you by Insurer with their final decision.